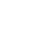
All You Wanted to Know About Cataract Surgery in Singapore

Cataract surgery – you’ve probably heard this mentioned numerous times before, or maybe someone you know might have just had an operation to have their cataracts removed!
If you’ve been diagnosed with cataracts, you would probably already have some understanding of what a cataract surgery procedure entails. However, the thought of having surgery performed on your own eye actually seems quite daunting, which is certainly understandable!
In this article, it addresses some common questions which patients often ask about cataracts and cataract surgery.
What is a cataract?
A cataract is an optically-degraded clouding and hardening of the normally clear crystalline lens of the eye. It gives rise to symptoms such as blurry vision, a faded appearance to objects, more difficulty seeing in dim light, glare and haloes.
Who is at higher risk for cataracts?
- Individuals who are older
In the majority of cases, cataracts occur as a result of just getting a bit older. The average age range of onset of cataracts is between 50 to 60 years of age.
- Individuals with medical or co-existing eye problems
Patients with diabetes or who are on long-term topical or oral steroids, or had prior eye trauma or eye surgery (e.g. vitrectomy), are all at higher risk of developing cataracts. Individuals with inflammatory eye disease are also predisposed towards earlier development of cataracts.
- Younger individuals can have cataracts too
Cataracts can occur in children, adolescents and young adults for various reasons — the most common being prior eye trauma. Younger individuals with cataracts may also have had them from birth, or have a family history of early-onset cataracts, which increases their risk for early cataract.
Those with a history of infection or inflammation in the eye, or other co-existing eye conditions such as pediatric glaucoma or retinal disease, are also more prone towards cataract development.
I have been diagnosed to have a cataract. Must I definitely have my cataract removed?


Where cataracts affect vision, this may give rise to general blurriness, reduced contrast where images appear more faded, or glare around lights at night.
It must be mentioned that the cataracts in some very fortunate patients may never reach the stage in their lives where they need to be removed. But once one develops trouble seeing clearly for everyday tasks and driving, it’s probably a good time to consider cataract surgery.
However, the flipside is if cataracts are left for too long, they become hypermature. Such cataracts are technically more challenging to remove in surgery. They can certainly still be removed safely, although the profile and degree of surgical risks will be slightly increased. Thus, it is recommended that once your eye doctor determines that your cataract is causing you a reduction in your visual quality or functioning, it probably is a good idea to think about having surgery.
The last consideration when cataract surgery may be recommended earlier rather than later is in patients with a structural narrowness of the fluid outflow passage in the eye. This is a structural abnormality that may progress in time to a form of glaucoma known as angle closure glaucoma. Here, cataract removal not only improves the vision, but also corrects the structural abnormality of the narrow outflow passage and reduces the risk of angle closure progression.
Cataract surgery sounds scary. What exactly happens during the procedure?
The main aim of cataract surgery is to restore and improve visual function by removing the optically degraded crystalline lens and to implant a clear artificial intraocular lens (IOL).
Modern cataract surgery is a minimally-invasive surgery utilizing small incisions. The procedure involves the use of ultrasound energy to emulsify the solid lens material of your eye (a procedure known as “phacoemulsification”), followed by placement of the IOL into the eye. “Phaco” refers to the energy involved and “emulsification” the mechanical disruption of the lens into smaller pieces.
Cataract surgery involves the following steps, all performed by your eye surgeon:
- A micro-incision is made just at the edge of the cornea to allow instruments access to the cataract.
- Using very fine forceps, an opening is made on the top surface of the capsular bag in order for the surgeon to gain access to the cataract, which resides in the capsular bag.
- The surgeon uses a phacoemulsification handpiece device placed through the corneal incision to break up the lens material.
- The broken up lens matter is removed from the eye by suction through the same phacoemulsification handpiece.
- An IOL, which is essentially an optically clear, artificial lens implant, is placed into the capsular bag, taking the place and function of the cataractous lens.
- The corneal wound is sealed without stitches.
I’ve heard of computer-assisted cataract surgery. What exactly does that involve?
Computer-assisted cataract surgery is a current technology that may improve the placement and alignment of a toric IOL during cataract surgery. Toric IOLs need to be perfectly and precisely aligned, in order to neutralize the corneal astigmatism intrinsic in your eye. A toric IOL misalignment of 12º could lead to a residual astigmatism that is 40% of the initial astigmatic power.
Computer-assisted cataract surgery involves a digital system that uses an eye tracker and intraoperative measurements to guide the eye surgeon towards placement of the toric IOL in the precise position to correct for astigmatism.
The alternative to using computer-assisted toric IOL placement is a manual marking system where the eye surgeon uses a manual marking device (e.g. a marking pen) to mark the cornea externally just before surgery, to indicate the position of alignment required for the toric IOL.
What is laser-assisted cataract surgery?
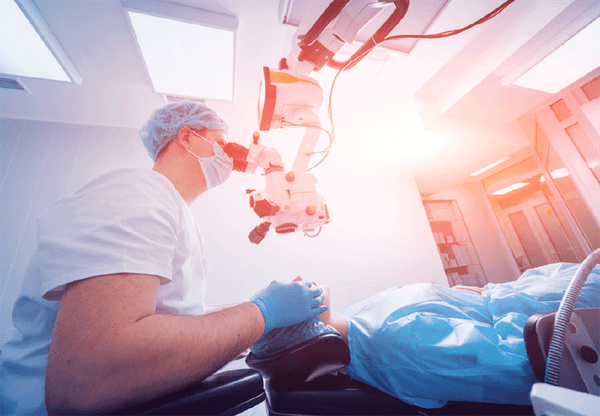
This is a more recently-developed technique of cataract removal, involving the use of a femtosecond laser for some of the steps in the cataract operation. The femtosecond laser automates the following steps in cataract surgery:
- Creation of minimally-invasive surgical access incisions into the eye
- Creation of the opening in the capsular bag to access the cataract
- Breaking up the cataract into more minute pieces
These steps are all performed in the same sitting by the femtosecond laser within a couple of seconds. The surgeon then has to subsequently proceed with the remaining steps of surgery in the usual manner, i.e., using a phacoemulsification handpiece device placed in your eye to remove the lens particles, and suctioning up these pieces.
Femtosecond laser-assisted cataract surgery may allow for more accurate IOL placement in the eye, may reduce the amount of phacoemulsification energy delivered, and may be advantageous to the surgeon in operating on more complex cataract cases.
However, these perspectives are not universally held by all surgeons.
Nevertheless, femtosecond laser cataract surgery may hold a slight benefit in patients in selected cases. As there is an increased surgical time and cataract surgery cost, it is certainly advisable that you discuss your specific need with your surgeon.
What are the Risks of Cataract Surgery?
Cataract surgery is a safe procedure and the vast majority of patients go on to enjoy much improved vision.
Your surgeon would be able to discuss the main risks of surgery with you prior to your surgery.
The vast majority of these complications such as dry eye, raised eye pressures, usual inflammation expected after cataract surgery, are relatively mild or transient and can be managed with medications. If appropriately managed, these do not impact on your visual outcome.
We will discuss 2 of the more important complications that patients undergoing cataract surgery should be aware of:
During the surgery, the capsular bag containing the cataract may be compromised. This is a complication termed “posterior capsule rupture”, and the risk is about 1%. In such cases, the original multifocal, trifocal or EDOF IOL may not be suitable, as these require an undamaged capsular bag for secure placement. A monofocal IOL may thus be implanted in these circumstances, not within the capsular bag, but on the surface of the bag instead.
If a posterior capsule rupture occurs, the visual recovery can potentially take slightly longer than usual. However, it is entirely possible that even with a capsular rupture, you can still achieve good quality vision, similar to if the capsular rupture did not occur.
In the months after surgery, some patients develop a thickening of the back surface of the capsular bag holding the artificial lens implant in place, giving rise to visual symptoms similar to that before cataract surgery, i.e. blurry vision, glare and haloes. Although the symptoms may raise some concern, this fairly benign condition, termed posterior capsule opacification (PCO), can be treated with a low-risk, routine clinic procedure known as YAG capsulotomy. PCO is sometimes termed “after-cataract”, and therefore mistakenly regarded as the return of the original cataract. Cataracts, once removed, do not reappear, however the development of PCO gives blurry vision and glare, which are similar to the symptoms of cataracts. Patients can expect that their sight returns to normal within a few hours after the YAG capsulotomy procedure.
What can I expect on the Day of surgery?
Before surgery
After arriving at the clinic, eye drops will be given to dilate the pupil in your eye (the one that will be operated on). Anesthetic eye drops will also be given to numb your eyes.
Most cataract surgery is performed under local anaesthetic. Some sedation may be given as well, to help you relax during the procedure. The vast majority of patients do very well for surgery under local anesthesia. Of course, general anesthesia is an option as well, but this is usually absolutely necessary for patients with unique circumstances, e.g. a bodily tremor limiting the ability to lie fully still in the operation.
During surgery
Your eye will first be cleaned with antiseptic just before the operation, following which, your face and torso will first be covered with a sterile drape so the surgical field stays clean. Being covered with a drape may certainly give some patients anxiety, and thus the sedation is important to take some of the anxiety edge off.
You would not need to worry too much about not being able to keep your eyes open, as the eye lids are supported with special micro-braces, so ensuring the eye stays open throughout the surgery. You would also not need to worry about your eye moving excessively during the procedure as local anesthetic is placed onto your eye, and throughout the surgery, with the phacoemulsification handpiece placed within, excessive eye movement is very unlikely.
From time to time, you might feel a cold sensation over your eye from the irrigating solutions used during the procedure, and also hear whirring noises from the phacoemulsification machine as it is doing its job. At some points in the surgery you may also feel some pressure on your eye, but there is usually no significant pain because your eye has been locally anesthetized.
Additionally, you may find the spotlight in front of you quite dazzling, and that your vision fluctuates as the surgery proceeds. When your cataract is completely removed, you will notice that your vision becomes suddenly quite blurry, and is restored only when your IOL implant is placed into your eye.
Overall, the surgery will be completed in approximately 15 to 30 minutes.
What can I expect after surgery?
Immediately post-surgery
After surgery, you will be asked to rest for anywhere between 1 to 2 hours, until you feel well enough to go home. Your surgeon may also check your eyes again before you leave, just to make sure that everything is in order.
It is very helpful to bring a pair of sunglasses with you, and also have a friend or relative who would be able to accompany you home. Your eye will feel tired and gritty for the rest of the day, so we advise you to stay at home and rest as much as possible, and to avoid too much hand-held electronic devices or television, at least for the first 1-2 days.
A few days to weeks post-surgery
At Day 1 after surgery, most patients will have about 70% to 80% of their final vision. Most patients have relatively good vision afterwards, but this vision will still be slightly misty and imprecise for about 2-3 days, and then gradually improve. Depending on what the vision was like before, you may notice a significant improvement in your vision in these early days. Complete recovery of vision usually occurs over the first month.
Topical steroid and antibiotic eye drops are prescribed usually for a duration of 1 month from the date of the surgery. You will also be given advice on specific activity restriction, such as to avoid getting water into your eyes, or cooking, for at least 2 weeks. Driving is best avoided until you are accustomed to your new vision, and after you have seen your eye doctor in the follow-up appointments to establish what your level of vision is.
You will find sunglasses helpful for the first week, especially as you are trying to adjust to your new vision, which will appear fairly bright and different from just a day before surgery!
Follow-ups with your surgeon post-surgery
Your doctor will review you the following day, and at 1 week and 1 month after the surgery. Fluctuations in vision and visual quality in the first month are fairly common, and are often due to dry eye, in addition to the usual post-operative recovery of inflammation in the eye. Thus treating dry eye and using steroids for inflammation would be important facets of cataract surgery aftercare.
Conclusion


The vast majority of patients go on to enjoy much improved vision. The advances in cataract surgery instrumentation and IOL technology now mean that your vision can be restored, and can additionally give you new-found vision over a range of distances.
In The Guide to Intraocular Lenses (IOLs) and Customized Cataract Surgery, it shares how the cataract surgery is customised according to your eye condition, and specific visual and lifestyle needs. He also explains how the various IOLs differ in this article
If your vision bothers you and is giving you significant trouble with your activities or driving, it may be that you have developed a cataract. Scheduling an eye examination with the ophthalmologist is an important first step to understanding your eye condition, safeguarding your vision, and to learn about potential treatment options.