The Guide to Intraocular Lenses (IOLs) and Customized Cataract Surgery

This is a continuation of our cataract surgery series, where in our first article, All You Wanted to Know about Cataract Surgery, we had discussed the surgical technique, pre-operative and post-operative care, and potential complications of cataract surgery.
In this article, we discuss how in modern cataract surgery, your eye surgeon can customize the surgery to your eye to suit your specific visual and lifestyle needs. This is done by way of specific pre-operative testing procedures, and also by selecting the most appropriate intraocular lens (IOL) for your eye!
What further tests do I need before cataract surgery?
Precision is of utmost importance in achieving the targeted visual outcome. By this we mean that if we targeted to make you without any refractive error (i.e. 0 diopters), or with very minimal refractive error, in your eye after surgery, we would want to be absolutely certain that we are able to achieve this. Thus, to obtain an in-depth, comprehensive assessment of your eye, and to effectively plan cataract surgery, your ophthalmologist would usually conduct several further tests.
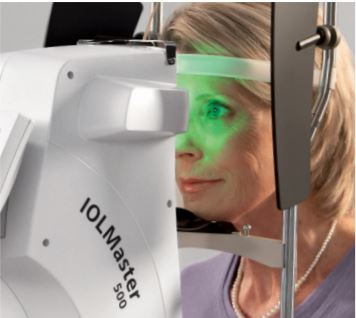 Biometry of your eye is absolutely necessary and uses sophisticated technology to quantify the length of your eyeball, your corneal curvature, and other important eye parameters, such as corneal width and the depth of the anterior chamber of your eye.
Biometry of your eye is absolutely necessary and uses sophisticated technology to quantify the length of your eyeball, your corneal curvature, and other important eye parameters, such as corneal width and the depth of the anterior chamber of your eye.
Mathematical calculations are then conducted based on these measurements to allow your surgeon to choose the intraocular lens (IOL) power most appropriate for your visual requirements.
Your eye surgeon may also require other tests to be done prior to cataract surgery, for example:
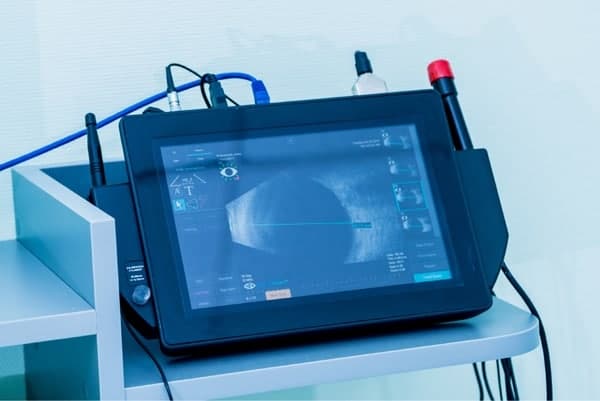
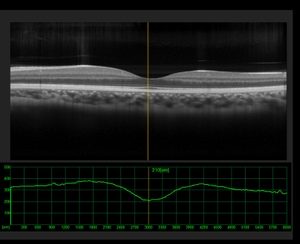 An optical coherence tomography scan of your retina may also be needed to assess for retinal issues prior to cataract surgery, particularly if you are a candidate for multifocal, trifocal, or extended-depth of focus (EDOF) IOLs. Such retinal issues must be identified before surgery as these can compromise the optical function of such IOLs.
An optical coherence tomography scan of your retina may also be needed to assess for retinal issues prior to cataract surgery, particularly if you are a candidate for multifocal, trifocal, or extended-depth of focus (EDOF) IOLs. Such retinal issues must be identified before surgery as these can compromise the optical function of such IOLs.
 A corneal topographic analysis may be required if you have had previous laser refractive surgery done, and if you may have misplaced your pre-refractive surgery corneal measurements. This will allow your surgeon to have information on your corneal curvature measurements to ensure that it corroborates with those measured with biometry.
A corneal topographic analysis may be required if you have had previous laser refractive surgery done, and if you may have misplaced your pre-refractive surgery corneal measurements. This will allow your surgeon to have information on your corneal curvature measurements to ensure that it corroborates with those measured with biometry.
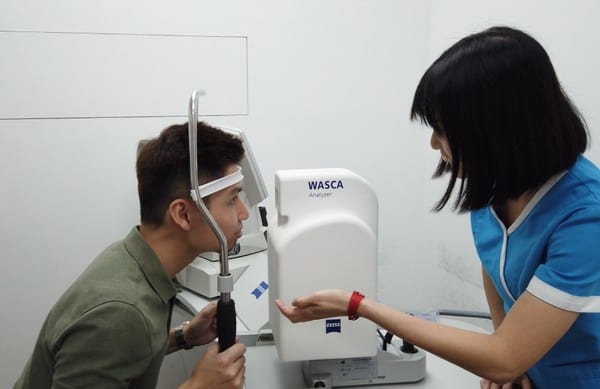 If you have had prior laser refractive surgery, a wavefront aberrometry may be needed to determine the level of optical aberrations in your cornea, especially if you are mildly symptomatic from these and may be considering specific IOL types.
If you have had prior laser refractive surgery, a wavefront aberrometry may be needed to determine the level of optical aberrations in your cornea, especially if you are mildly symptomatic from these and may be considering specific IOL types.
What types of intraocular lenses are there for placement during cataract surgery?
An intraocular lens (IOL) is a clear plastic disc-like implant that is placed into the capsular bag of the eye to take on the optical function of the natural crystalline lens.
The IOL selected for your eye is of a specific prescription and customized to your eye to allow you the most optimal vision and visual quality, based on your profile of vision-related activities.
A wide array of intraocular lenses are available for implantation, although the specific type of IOL that your surgeon may recommend will depend on certain parameters of your eye structure, your lifestyle needs, hobbies, driving habits, and desire for spectacle-freedom over a range of viewing distances.
Broadly speaking, viewing distances are classified into 3 main categories: distance (at 100 cm and beyond), intermediate (about 66 cm to 80 cm), and near (about 33 cm)
There are 3 main groups of intraocular lens options available for patients:
- Monofocal Aspheric IOLs
Monofocal IOLs, as the name suggests, have a single focus point. In the majority of individuals who have monofocal IOLs placed, the specific prescription of the IOL is customized to a distance focal point, and so allow good distance vision.

What your vision might look like after cataract surgery with monofocal IOL placement
These IOLs offer excellent quality of distance vision with very minimal to no glare* or halos, compared with multifocal, trifocal, or extended-depth of focus (EDOF) IOLs. If you are happy with using glasses for near or intermediate distance activities, these lenses provide very good quality distance vision, e.g. for driving in the day and night.
However, you would very likely still need spectacle correction for near or intermediate distance activities, e.g. using glasses for reading, using the computer, or watching television.

*Glare refers to the indistinct edge of fuzzy light, observed when one looks at a point source of light, e.g. a street lamp at night. Halos are additional rings of light seen when one looks at a point light source. Starbursts appear as radially scattered light.
Monofocal aspheric IOLs may also be implanted and customized to a near focus, instead of a distance focus. This would allow near objects to be in focus, whilst distance objects would be out of focus. Such refractive targeting is most commonly performed to achieve monovision correction in a patient.
What is monovision correction?
Some individuals are able to use one eye for distance viewing, and another for near, in a state known as “monovision”. This strategy is sometimes employed in appropriate individuals who undergo cataract surgery with monofocal IOLs.
In monovision correction, the prescription of the monofocal IOLs are optimized such that the IOL in one eye allows for good distance vision, while the IOL in the other eye is optimized for good near vision. Usually, the dominant eye is corrected for distance vision, and the non-dominant eye is corrected for near vision.
This may feel awkward at first for individuals who are not already using monovision with their current spectacle or contact lens. Therefore, for individuals who are keen to consider monovision correction, suitability must first be tested with a trial using contact lenses to simulate what this feels like for the individual.
The downside to monovision is that it reduces one’s appreciation of space and depth, and so individuals may observe that objects appear to be less 3-dimensional than what they really are.
- Multifocal, Trifocal & Extended Depth of Focus (EDOF) IOLs
Multifocal IOLs (which are really “bifocal” IOLs) aim to allow the individual to have both good distance vision and near vision without spectacles.
Trifocal IOLs, as the name suggests, target distance, intermediate and near vision.
Extended depth-of-focus (EDOF) IOLs address some of the fall-off in vision within specific viewing ranges with the bifocal or trifocal IOLs. For instance, the reduced vision between distance and intermediate distances may be an issue for some individuals. EDOF IOLs provide a more gradual transition in vision between these distances.

What your vision might look like with a trifocal IOL
While the ability to see well without spectacles at specific distances, or over a range of distances, are certainly advantages of such IOLs, it must be stressed that patients with these IOLS implanted MUST trade off accepting some degree of reduced contrast (i.e. images appear dimmer or less vibrant than expected), as well as a much higher likelihood of appearance of glare and halos around lights at night, than with monofocal IOLs.
These symptoms usually get better with time as individuals tend to adapt to the new visual quality, but nevertheless these visual phenomena will still be apparent from time to time. Within the group of such IOLs, EDOF IOLs may cause less glare and haloes than trifocals, and may thus be more suited for individuals desiring spectacle-freedom who wish to drive at night.
Such IOLs can be implanted in the majority of patients with normal eyes, including patients who have had previous laser refractive surgery (i.e. LASIK or PRK).
However, patients with underlying retinal diseases involving the macula, or glaucoma, are not suitable candidates for such IOLs because these eye diseases compromise the optimal optical functioning of such IOLs.
Lastly, it must also be mentioned that healthy tear production is a very important factor that also affects the optimal visual performance of such IOLs. Patients with dry eyes can still be considered for these IOLs. However, adequately moisturizing dry eyes both before and after the cataract surgery procedure will be very important in this group of patients.
- Toric IOLs
These lenses are used to correct corneal astigmatism (“san guang”). Astigmatism is a specific type of refractive error that arises from the cornea being more curved along one plane, than in the rest of the cornea. Just as there is a great variety of heights and weights amongst different people in the population, corneal curvature likewise varies quite a bit amongst different people.
In order to customize the IOL option specific to your eye, an IOL neutralizing the corneal astigmatism is required. Usually, if the corneal astigmatism is less than 0.5 diopters, you may not need a toric IOL.
Monofocal, multifocal, trifocal and EDOF IOLs come with toric lens options as well.
Your ophthalmologist would be able to advise you on the need for a toric lens option to correct your corneal astigmatism.
Will I Still Need Glasses After Cataract Surgery?
Whether you need glasses after cataract surgery really depends on the type of IOL implant you choose. Each IOL type has a unique profile of visual capabilities, and you will have to discuss with your ophthalmologist regarding the type of IOL that works best for you.
Here is a quick summary of the most commonly-implanted IOLs (i.e., monofocal, trifocal, and EDOF IOLs), as we have discussed in point 2 above.
| Monofocal IOLs | Trifocal IOLs | EDOF IOLs | |
|---|---|---|---|
| What it does | Targets focus for a specific distance. Usually customized for distance vision. | Targets focus for distance, intermediate and near distances, but the intervening regions are often defocused | Provides a continuous focussing range between specific distances |
| Visual capabilities |
|
|
|
| Benefits |
|
|
|
| Drawbacks | Reading glasses are needed for near vision tasks such as reading, cooking and intermediate distance activities, such as television viewing or working on the computer. |
|
|
| Who may be suitable | People who do not mind wearing reading glasses |
|
|
| Who would not be suitable |
|
Patients with macular problems in their retina, or glaucoma, or amblyopia (lazy eye) |
Those with significant astigmatism (usually more than -0.50 D) would usually require toric IOLs. Monofocal, trifocal and EDOF IOLs all come with toric options. For those who have had trifocal and EDOF IOLs, reading is generally encouraged under good lighting conditions, e.g. using a reading lamp.
Conclusion
Importantly, there should not be a “one-size-fits-all” approach for your own cataract surgery! The decision to undergo cataract surgery is certainly one that requires an in-depth discussion with your eye surgeon concerning your occupational, social and lifestyle needs, and desire for spectacle-independence.
There are a range of IOL options available currently, with the potential to allow you to achieve spectacle-independence at various distances, and afford you improved quality of life. The discussion with your eye surgeon should also address your expectations, as well as for you to gain an understanding of the potential benefits of each IOL option, and compromises that you inevitably will have to trade-off in return for greater spectacle-freedom.
Therefore at present, there is no one “perfect IOL”, one which offers uncompromised visual quality without the optical effects of glare and halos, and at the same time providing good vision at all distances, and under dim lighting conditions as well. Until we can postpone our own cataract surgery far into the future when such an ideal IOL may have been invented, this goal will remain the holy grail of cataract surgery!
Request for an appointment.

Tel: +65 6836 1000
Whatsapp: +65 9843 1000
For general enquiries and appointment only
Email: [email protected]
Monday to Friday: 9am to 6pm
Saturday: 9am to 4pm
*Last Registration Time 2pm
Sunday & PH: Closed
Comment (1)
Leave your thought here
You must be logged in to post a comment.












aliessia
I think I have a lot to offer. Maybe it’s my voice that turns live cams models you on or maybe it’s something else. But see for yourself.